5.5 Orbit
Introductory Comments
The orbit examination is one of the most difficult to perform under examination conditions. A large number of potential manoeuvres and measurements need to be performed. It is important that the examiner be comprehensive and systematic, yet flexible enough to tailor their exam to the patient being examined. Avoid verbalising a long list of negatives (e.g. “there is no hypertelorism”) that will be of little interest to an examiner. Most orbital patients will either have inflammation (most commonly thyroid orbitopathy) or an orbital tumour (including vascular, cystic and neoplastic lesions). Primary objectives of the orbit examination include establishing a differential diagnosis, assessing optic nerve integrity and documenting baseline findings for later comparison.
The worse eye is usually the affected one (may be amblyopic).
If the patient wears spectacles, remove these prior to further inspection / palpation. Look at the whole patient for clues (e.g. syndromes).
- Eyelids
- Ptosis or lid retraction (superior scleral show)
- Upper and lower lid swelling in TED
- Periocular soft tissue inflammation
- Proptosis / enophthalmos
- Describe whether this is unilateral or bilateral, axial or non-axial and whether it is pulsatile
- Inferior scleral show is a very sensitive early sign of proptosis
- Consider the possibility of pseudo-proptosis
- Dystopia, hypertelorism / telecanthus, strabismus
- Corneal light reflexes may assist in the detection of these, but often they can be detected just with careful inspection
- Dystopia = Abnormal position (of the eye), such as hypoglobus (in an orbital floor fracture or superior orbital mass)
- Hypertelorism = Increased distance between eyes (orbits), such as in craniosynostoses
- Telecanthus = Increased distance between the medial canthi (> 35mm), such as in blepharophimosis syndrome
- Pupils (anisocoria)
- Face / neck
- Look for neck (thyroidectomy) scars, goitres and other masses. The patient may have been instructed to wear a scarf which candidates should ask to be removed
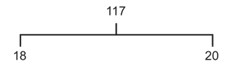
Hertel exophthalmometry measures the distance between the lateral orbital rim and the corneal apex. Proptosis of greater than 22mm or an asymmetry of greater than 2mm between is significant. Note the distance between the lateral orbital rims to allow subsequent measurements to be comparable.
Performing Exophthalmometry
Tell the patient that “I am going to place this (exophthalmometer) on the corner of your eyes”. Feeling for the lateral orbital rims before positioning the exophthalmometer prevents startling the patient or causing them pain (a certain fail in exams). This also allows for palpation in case of lateral wall orbital decompression in thyroid orbitopathy. Widen the exophthalmometer until it just rests on the lateral orbital rims. Close your right eye and position this in front of the patient’s right eye. Tell the patient to “look at my closed eye”. Using your left eye, adjust your head position so that the line on the exophthalmometer is appropriately centered (to eliminate parallax error). Read off the position of the corneal apex on the graticule. Repeat for the patient’s left eye by positioning your closed left eye in front of it and reading the measurement with your right eye.
Measuring Dystopia
Under the time pressure of exam conditions there is often insufficient time to measure dystopia, but if this is requested the following process should be followed. Place a horizontal ruler centred on the nose, passing in front of the lateral canthi. Measure the horizontal distance between the midline and the corneal reflex and the vertical displacement from this plane.
Warn the patient that “I am going to feel around your eyes. Please close your eyes”.
Orbital Rim / Lacrimal Sac
- Use your thumbs and feel for bony steps (fractures, orbital decompression for thyroid orbitopathy) and masses
Fornices
- Inferior: Ask the patient to “look up” and look for masses or inflamed inferior recti
- Superior: Ask the patient to “look down” and look for masses including enlarged lacrimal glands ask the patient to look “down and left / right”
Retropulsion
- Ask the patient to “gently close your eyes” and warn them that you are going to “gently press on their eyes”. Use both thumbs and press on each eye one at a time. Increased orbital resistance is found in diffuse inflammatory disease and discrete mass lesions. Feel for thrills (carotid cavernous fistulae).
Auscultation
- A stethoscope sitting beside the patient in an exam is a subtle hint that it should be used! Whilst the patient still has their eyes closed, place the diaphragm of a stethoscope on their closed eyes, then ask them to “open your eyes”. This relaxes orbicular oculi tone of the eyelid still closed beneath the diaphragm. Listen for a bruit (carotid cavernous fistulae).
Lymphadenopathy
- Palpate for lymphadnenopathy (especially preauricular, submandibular and supraclavicular)
Facial Sensation (Cranial Nerve V)
- Using your finger, check facial sensation in the three divisions of the trigeminal nerve (ophthalmic, maxillary, mandibular). Corneal sensation (CNV1) will not be permitted in most exams but can be requested. Ask the patient to “Say “yes” when you feel me touch your face” and check for symmetry across the vertical midline. Loss of V1 sensation suggests an intraorbital or superior orbital fissure abnormality, whereas loss of V2 sensation suggest perineural spread of a skin tumour or previous orbital floor fracture.
Valsalva Manoeuvre
- Ask the patient to close their mouth, pinch their nose and “blow out” to “pop your ears”. Elicitation of proptosis is seen with orbital varices.
This is the most important parameter measured in an orbital exam. Ensure you do not run out of time to check these.
Pupils
- Using a direct or indirect ophthalmoscope light check for direct and consensual reflexes and the presence / absence of a relative afferent pupillary defect (RAPD). You must request the lights be turned off before checking for a RAPD.
Redness Saturation
- Redness saturation is determined by presenting a red target (such as a red card) to each eye in turn and asking the patient to compare the redness between each as a percentage from 1 to 100. It is faster if you cover the patient’s other eye rather than getting them to do it themselves.
Brightness Saturation
- Brightness saturation is determined by presenting a uniform light source (such as from a direct or indirect ophthalmoscope) to each eye in turn and asking the patient to compare the brightness between each as a percentage from 1 to 100. Asymmetry in redness and brightness saturation is suggestive of optic nerve dysfunction.
Visual Fields to Confrontation
Optic Disc Appearance
Under exam conditions there is rarely sufficient time to perform cover testing. Proceed to examining ocular rotations with an “H” pattern. With the eyes straight, check upgaze then downgaze, making note of the presence / absence of “lid lag” (the upper lid lagging behind the speed of the depression of the globe, as seen in thyroid orbitopathy)
Previous
5.4 Ptosis
All rights reserved. No part of this publication which includes all images and diagrams may be reproduced, distributed, or transmitted in any form or by any means, including photocopying, recording, or other electronic or mechanical methods, without the prior written permission of the authors, except in the case of brief quotations embodied in critical reviews and certain other noncommercial uses permitted by copyright law.
Vitreoretinal Surgery Online
This open-source textbook provides step-by-step instructions for the full spectrum of vitreoretinal surgical procedures. An international collaboration from over 90 authors worldwide, this text is rich in high quality videos and illustrations.