6 Strabismus
6.8 Brown Syndrome
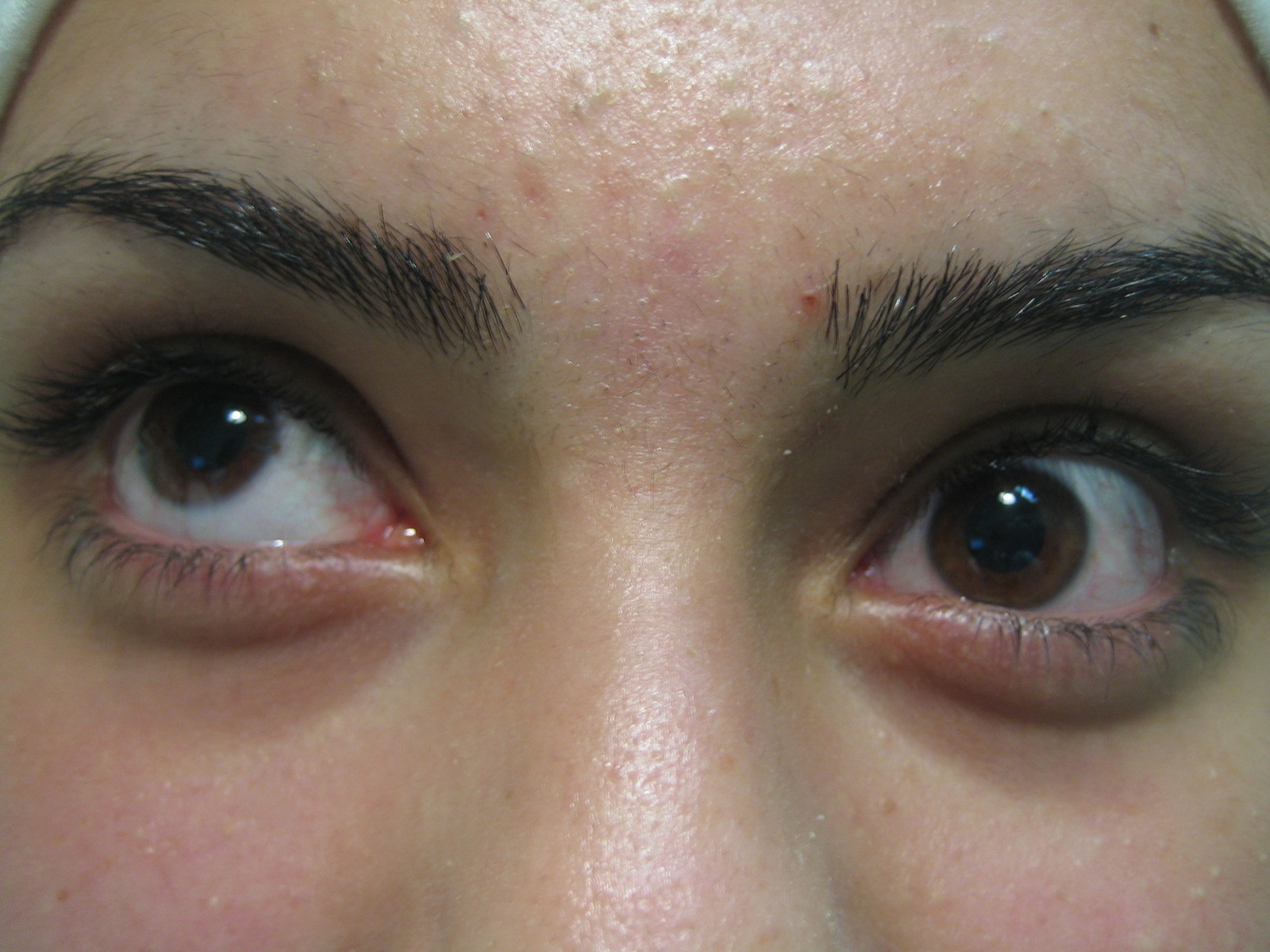
- Hallmark: Syndrome of deficient elevation in adduction due to restriction of the superior oblique (SO) tendon or trochlea-tendon complex
- The limitation in elevation improves to normal or near normal elevation in abduction
- Also known as Superior Oblique Tendon Sheath syndrome
Congenital (no Diplopia Suppression)
Idiopathic
- Mild (limited elevation in adduction)
- Moderate (+ downshoot in adduction)
- Severe (+ hypotropia in primary)
Acquired (May Get Diplopia)
- Trauma to the trochlea or SO tendon (e.g. “canine tooth syndrome”)
- Inflammation of the trochlea or SO tendon (rheumatoid arthritis, sinusitis, scleritis)
Downshoot in Adduction
Hypotropia in Primary
Surgery
Mild
Downshoot in Adduction
No
Hypotropia in Primary
No
Surgery
No
Moderate
Downshoot in Adduction
Yes
Hypotropia in Primary
No
Surgery
No
Severe
Downshoot in Adduction
Yes
Hypotropia in Primary
Yes
Surgery
No
- Amblyopia is rare
- Abnormal head position- chin up, head turn to the opposite side
- Hirschberg (Pupil margin = 15°, Iris margin = 30°)
- (Lids normal)
- (Pupils normal)
- Inspect for trauma around the trochlea
- Often straight or small hypotropia in primary (congenital)
- Acquired usually have larger hypotropia
- ~90% Unilateral
- Hallmark: Limited elevation in adduction, which improves to normal or near normal elevation in abduction. Most easily demonstrated by bringing the eye from abduction to adduction in upgaze and seeing it fall (the “falling eye sign”)
- No improvement with ductions
- No “superior oblique overaction” (SOOA)
- V pattern
- Feel for trauma, inflammation (in acquired Brown syndrome)
- Positive
- Tested by feeling for a click on elevation in adduction.
- Accentuated in this position by retropulsion
Browns
IO Palsy (rare)
Damage to inferior division of CNIII
Monocular Elevation Deficit
Laterality
Browns
90% Unilateral
IO Palsy (rare)
Damage to inferior division of CNIII
Unilateral
Monocular Elevation Deficit
Unilateral
Primary
Browns
Straight or hypotropic (usually <10Δ)
IO Palsy (rare)
Damage to inferior division of CNIII
More hypotropia (usually >10Δ)
Monocular Elevation Deficit
Hypotropia
Adduction
Browns
± Downshoot
Limitation of elevation in adduction
No improvement with ductions
IO Palsy (rare)
Damage to inferior division of CNIII
± Downshoot
Limitation of elevation in adduction
Improvement with ductions
Monocular Elevation Deficit
Limited elevation in both adduction and abduction
“SOOA”
Browns
No
IO Palsy (rare)
Damage to inferior division of CNIII
Yes
Monocular Elevation Deficit
No
Alphabet pattern
Browns
V pattern
IO Palsy (rare)
Damage to inferior division of CNIII
A pattern
Monocular Elevation Deficit
No alphabet pattern
Forced duction
Browns
Positive
IO Palsy (rare)
Damage to inferior division of CNIII
Negative
Monocular Elevation Deficit
Normal or positive
FGT may show weak SR
Trochlear
Browns
May feel click
IO Palsy (rare)
Damage to inferior division of CNIII
Normal
Monocular Elevation Deficit
Normal
- Limitation of elevation in adduction and abduction
Previous
6.7 Duane Syndrome
All rights reserved. No part of this publication which includes all images and diagrams may be reproduced, distributed, or transmitted in any form or by any means, including photocopying, recording, or other electronic or mechanical methods, without the prior written permission of the authors, except in the case of brief quotations embodied in critical reviews and certain other noncommercial uses permitted by copyright law.
Vitreoretinal Surgery Online
This open-source textbook provides step-by-step instructions for the full spectrum of vitreoretinal surgical procedures. An international collaboration from over 90 authors worldwide, this text is rich in high quality videos and illustrations.