5.7 Oculoplastic Differential Diagnoses
Contents
Vascular
- Lymphangioma
- CCF
Endocrine
Thyroid Eye Disease
Infective / Inflammatory
- Orbital cellulitis
- Bacterial infections cause profound acute inflammation
- Fungal infections can present more insidiously. Always exclude mucormycosis in diabetic patients with orbital cellulitis
- Masquerading infections (TB, syphilis)
- Bacterial infections cause profound acute inflammation
- Orbital inflammatory diseases
- Sarcoid
- GPA / Wegeners or other vasculitis disorders
- IgG4-related disease
- Sarcoid
Neoplasia
- Aggressive neoplasms can cause or mimic acute inflammation
- Lymphoma often presents as subacute or chronic inflammation
Other
- Ruptured dermoid cyst
- Medication-related
- Bisphosphonates
Increased Orbital Volume
- Orbital floor fracture
- Bony remodelling (silent sinus syndrome)
- Absence of greater wing of sphenoid (Neurofibromatosis type 1)
Orbital Tissue Atrophy
- Age related involutional changes
- Scirrhous metastasis (breast cancer)
- Post-Surgical (fracture repair, blepharoplasty, enucleation)
- Lid Scleroderma
- Hemifacial atrophy
- Prostaglandin Associated Periorbitopathy
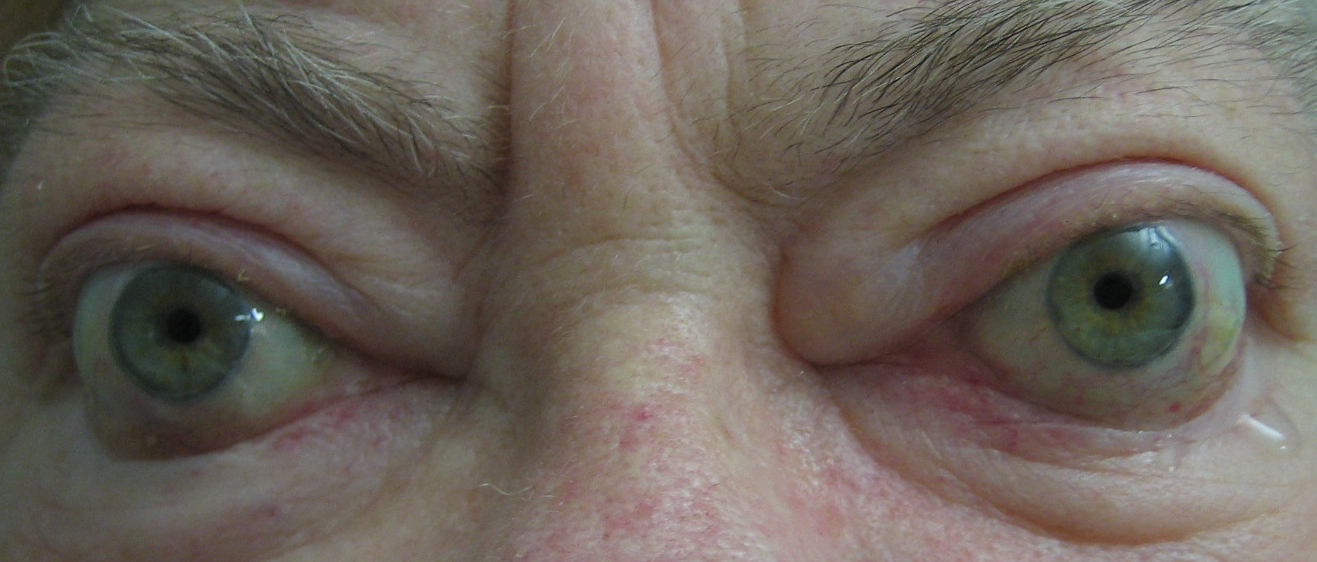
Contralateral Exophthalmos
Globe Retraction
- Duane’s Syndrome
- Convergence-Retraction nystagmus (Parinaud’s syndrome)
Tendon Sparing
Thyroid Eye Disease
Tendon-Involving
- Idiopathic Orbital Inflammatory Disease
- Carotid-Cavernous Fistula
- Neoplasia (lymphoma, metastasis)
Neurogenic
- MGJW
- Aberrant CN III Palsy
- Duane’s Syndrome
- Parinaud’s Syndrome
- CN VII Palsy
- Phenylepherine
Myogenic
Thyroid Eye Disease
Mechanical
- Any causes of proptosis
- Buphthalmos
- Overcorrection following ptosis repair
- Hypogonadism
- Hypothyroidism
- Scleroderma
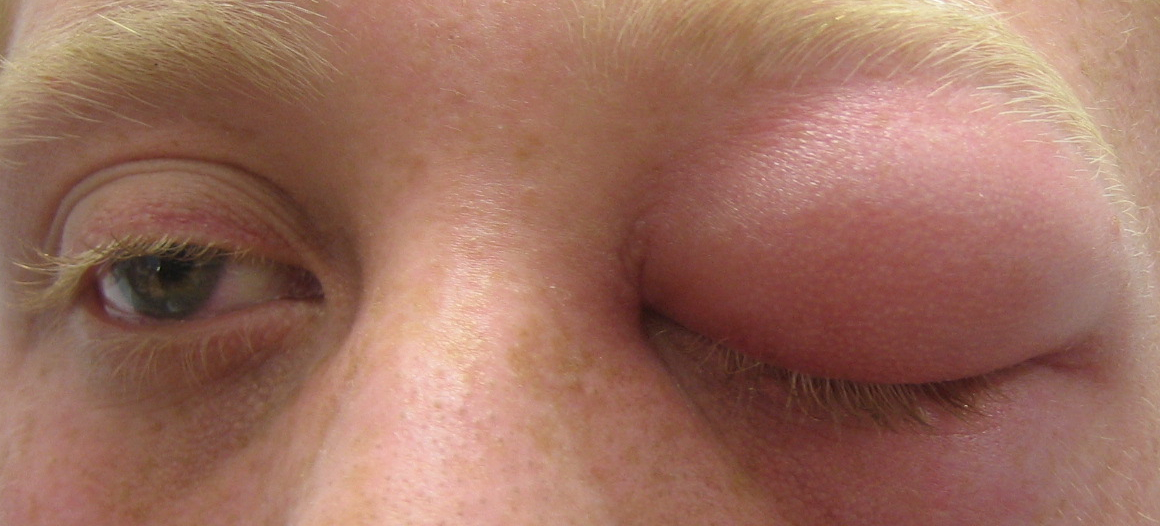
Dacryoadenitis
- Infective
- Viral (mumps, EBV, influenza, VZV)
- Bacterial
- Inflammatory
- IOID
- Sarcoid (Mikulicz syndrome)
- Tuberculosis
- Granulomatous polyangiitis (Wegener’s)
- Polyarteritis nodosa
Neoplastic
- Benign
- Pleomorphic adenoma
- Plexiform Neurofibroma
- Malignant
- Pleomorphic adenocarcinoma
- Adenoid cystic carcinoma
Others
- Dermoid Cyst
- Lipodermoid
Local
- Blepharitis
- Tumour
- Radiation Therapy
Dermatological
- Alopecia
- Psoriasis
- Severe Rosacea
Systemic
- Hypothyroidism
- SLE
- Syphilis
- Leprosy
Others
- Iatrogenic
- Trichotilomania
“MINT”
- M igraine
- I nflammatory and I nfective
- Inflammtory: Tolosa hunt, IOID, GCA
- Infective: Orbital Abscess, mucormycosis, post-herpetic neuralgia
- N eoplastic
- T rauma (orbital fracture)
“VEIN-O”
- M igraine
- I nflammatory and I nfective
- Inflammtory: Tolosa hunt, IOID, GCA
- Infective: Orbital Abscess, mucormycosis, post-herpetic neuralgia
- N eoplastic
- T rauma (orbital fracture)
V ascular
- Orbital Varix
- Carotid Cavernous Fistula (CCF)
E ndocrine
Thyroid Ophthalmopathy
I nfective / Inflammatory
- Idiopathic Orbital Inflmmatory Disease (IOID)
- Orbital Cellulitis
N eoplastic
- Cavernous haemangioma
- Lacrimal gland (pleomorphic adenoma, Ca)
- Optic Nerve (glioma)
- Meningioma
- Neurofibroma
- Lymphoma
- Sphenoid wing meningioma
- Metastases
- Invasion by sinus tumours (nasopharyngeal and maxillary cancer)
O ther
- Dermoid Cyst
- Sinus mucocele
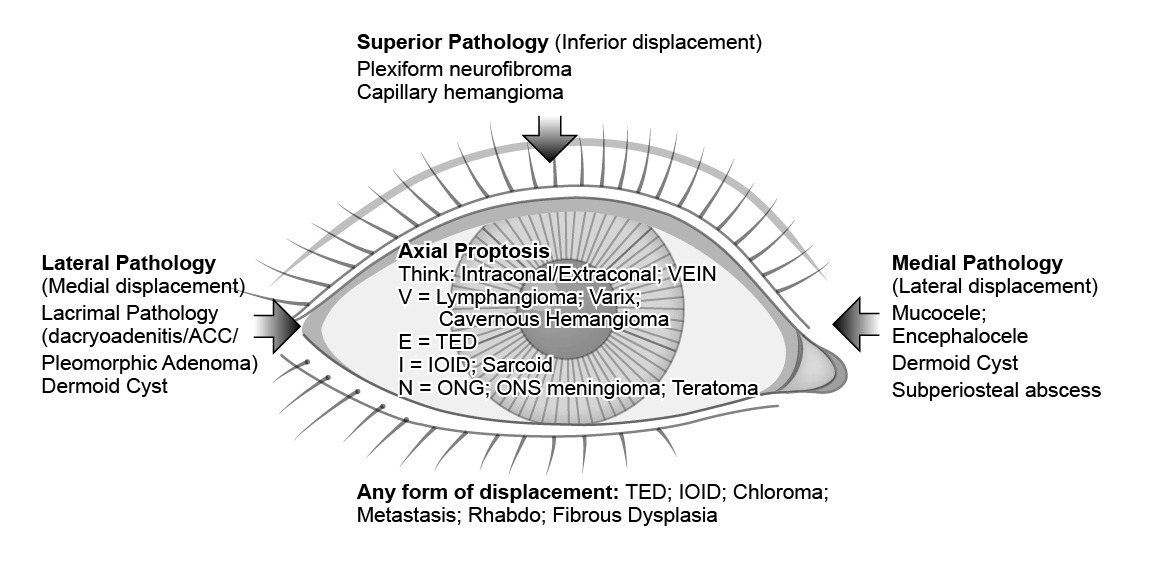
When approaching proptosis, these categories will help differentiate the various pathologies:
- Axial vs non-Axial proptosis
- Time course (acute vs subacute vs chronic vs intermittent)
- Adult or Childhood onset
The appearance of proptosis (not true proptosis):
- Ipsilateral upper eyelid retraction or contralateral ptosis
- Contralateral enophthalmos
- Enlarged globe (e.g. high myopia, buphthalmos)
- Asymmetrical orbits (craniofacial anomalies)
- Carotid-cavernous fistula
- Sphenoid wing dysplasia (NF-1)
- AV malformation
- Trauma (Orbital Roof fracture)
Previous
5.6 Thyroid Eye Disease
Next
6.0 Introduction
All rights reserved. No part of this publication which includes all images and diagrams may be reproduced, distributed, or transmitted in any form or by any means, including photocopying, recording, or other electronic or mechanical methods, without the prior written permission of the authors, except in the case of brief quotations embodied in critical reviews and certain other noncommercial uses permitted by copyright law.
Vitreoretinal Surgery Online
This open-source textbook provides step-by-step instructions for the full spectrum of vitreoretinal surgical procedures. An international collaboration from over 90 authors worldwide, this text is rich in high quality videos and illustrations.