7 Neuro-Ophthalmology
7.1 Cranial Nerve III (Oculomotor) Palsy
7.2 Cranial Nerve IV (Trochlear) Palsy
7.3 Cranial Nerve VI (Abducens) Palsy
7.4 Cranial Nerve VII (Facial) Palsy
7.5 Optic Nerve Function
7.6 Visual Fields to Confrontation
7.7 Pupils
7.8 Horner’s Syndrome
7.9 Nystagmus
7.10 Neuro-Ophthalmic Differential Diagnoses and Aetiologies
7.10 Neuro-Ophthalmic Differential Diagnoses and Aetiologies
- Bi-nasal Hemianopia
- Centrocaecal Scotoma (Bilateral)
- Chiasmal Disease
- Gaze Palsies
- Idiopathic Intracranial Hypertension (Pseudotumour cerebri) – Mimics to Exclude
- Light-Near Dissociation
- Miosis
- Mydriasis
- Myasthenia Gravis
- Non-Arteritic Anterior Ischaemic Optic Neuropathy - NAION (Risk Factors)
- Optic Atrophy
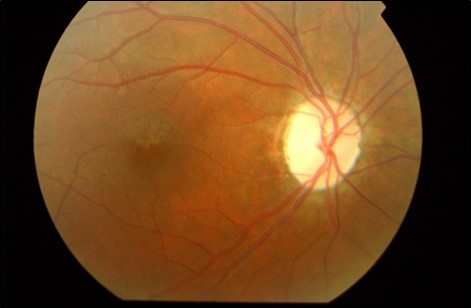
- Optic Disc Cupping
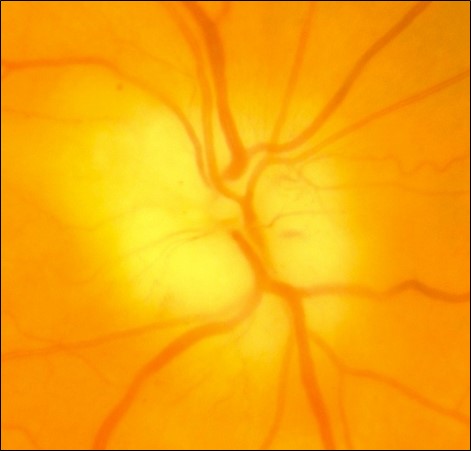
- Optic Disc Swelling
- Optic Disc Swelling (Bilateral)
- Optic Neuropathy (Causes)
- Dermatochalasis
- Tilted discs, Optic disc drusen
- Bilateral sectoral retinitis pigmentosa, temporal retinoschisis, vigabatrin toxicity
- Chronic raised intra-cranial pressure
- Syphilis
- Compression of lateral optic nerve / chiasm by an ICA aneurysm
“THONG”
- Toxic
- Alcohol
- Hereditary
- Leber’s hereditary optic neuropathy
- Optic neuritis
- Nutritional
- Vitamin B12 deficiency
- Glaucoma
- Acute angle closure glaucoma
- Neoplasia
- Pituitary macroadenoma
- Craniopharyngioma
- Children: Dwarfism, delayed sexual development, obesity
- Adults: Visual loss
- Meningioma
- Tuberculum sellae, sphenoidal ridge
- Glioma
- Pituitary macroadenoma
- Vascular
- Aneurysm
- CVA
- Cystic
- Sinus mucocele
- Inflammatory
- Multiple sclerosis
In most supranuclear motility disease saccades are affected first, then pursuit, then the vestibulo-ocular reflex.
Control
- Horizontal eye movements
- Frontal Eye Fields: Generates horizontal saccade to the opposite side
- Occipital: Generates horizontal pursuit to the same side
- PPRF: Enacts horizontal gaze to the same side
- (Ipsilateral CNVI, Contralateral CNIII)
- Vertical eye movements
- Generated from the Rostral Interstitial Nucleus of the MLF (riMLF, midbrain) and the Interstitial Nucleus of Cajal (INC)
Aetiology of Gaze Palsies
- CVA
- Tumour
- MS
- Infection (encephalitis)
- Trauma
- Hydrocephalus
- Drugs
- Conditions causing vertical gaze palsies:
- Parinaud’s (dorsal midbrain) syndrome
- Young male: Pinealoma, Craniopharyngioma
- Young female: MS
- Elderly: CVA
- Parinaud’s (dorsal midbrain) syndrome
- Progressive Supranuclear palsy (Steele-Richardson-Olszewski)
Progressive Supranuclear Palsy versus Parkinson’s Disease
Progressive Supranuclear Palsy
Parkinson’s Disease
Mask Like Facies and ↓ Blink Rate
Progressive Supranuclear Palsy
Usually a more worried expression
Parkinson’s Disease
Ophthalmoparesis
Progressive Supranuclear Palsy
- Supranuclear paralysis of down then upgaze / horizontal (slow vertical saccades BUT good Doll’s head)
- ± Convergence insufficiency
- Eyelid apraxia
Parkinson’s Disease
- Ophthalmoplegia is usually a mild feature
- Blepharospasm / apraxia lid opening
- Convergence insufficiency
- Dry eye, blepharitis
Pseudobulbar Palsy
Progressive Supranuclear Palsy
(early dysarthria / dysphagia)
Parkinson’s Disease
±
Postural Instability With Falls
Progressive Supranuclear Palsy
(early, fall back)
Parkinson’s Disease
± (late, fall forwards)
Rigidity
Progressive Supranuclear Palsy
Parkinson’s Disease
Bradykinesia
Progressive Supranuclear Palsy
Parkinson’s Disease
Tremor
Progressive Supranuclear Palsy
Parkinson’s Disease
Prognosis
Progressive Supranuclear Palsy
Worse (death within 10 years)
Parkinson’s Disease
Better
L-DOPA
Progressive Supranuclear Palsy
Unresponsive
Parkinson’s Disease
Responsive
- Diseases
- Chronic lung disease / Obstructive sleep apnoea, anaemia, renal failure, hypothyroidism, Addison’s disease
- Drugs “OATS”
- Oral contraceptive pill (causes weight gain and dural venous thrombosis)
- Vitamin A (e.g. acne cream)
- Tetracyclines
- Steroids (esp. withdrawal), Cyclosporine
“ABCD”
- Adie’s tonic pupil, Argyll-Robertson pupil
- Bilateral severe loss afferent light input into BE (retinas, ONs, chiasm)
- CN III aberrant regeneration
- Dorsal midbrain syndrome, myotonic dystrophy, diabetes
Anisocoria worse in dark – ‘4 P”
- Pancoast tumour (Horners)
- ****Prostitute (Argyll Robertson pupil)
- Pilocarpine
- Posterior synechiae
- (Old Adie’s pupil)
Anisocoria worse in light – “4 T”s
- Tonic pupil
- Third nerve palsy
- Tropicamide (dilating drops)
- Trauma
Ocular Myasthenia
- Mitochondrial encephalomyopathies (CPEO, Kearns-Sayre, MELAS)
- Oculopharyngeal dystrophy (AD)
- Thyroid eye disease
- CN palsy
- Other causes of ptosis
Generalised Myasthenia
Miller Fisher Syndrome (Variant of Guillain-Barré Syndrome)
- Triad: Ophthalmoplegia + Ataxia + Areflexia.
- Anti-ganglioside complex antibodies (Anti-GQ1b), ↑ CSF protein
Myotonic Dystrophy
- Diplopia rare, no fatigue / diurnal variation
- Myotonic handshake
- Christmas tree cataracts
- Frontal balding
Eaton-Lambert Myasthenic Syndrome
- Ocular / bulbar involvement rare except for ptosis
- Muscle strength increases after exercise
Botulinum
- Dilated pupils (doesn’t occur in MG)
“Disc at risk” (small cup) +
- Old age
- Atherosclerosis
- Hypertension
- Nocturnal hypotension (often on awakening)
- Hypercholesterolaemia
- Diabetes
- Smoking
- Obesity
- Obstructive sleep apnea
- Anaemia
- Vasculitis
- Hyperviscosity
- Thrombophilia
- Drugs
- Sildenafil
- Amiodarone
- Cataract surgery
- Performing cataract surgery when the fellow eye has already had an NAION has an absolute risk of around 50% of causing an NAION in the operated eye
- The risk of NAION being caused by cataract surgery in an eye that is “at risk” (but with no history of NAION in the fellow eye) is unclear
- Optic disc drusen
Non-Arteritic versus Arteritic Ischaemic Optic Neuropathy
Non-Arteritic (NAAION)
Arteritic (AAION)
Epidemiology
Non-Arteritic (NAAION)
90%
45-65yrs
M=F
Arteritic (AAION)
10%
> 65yrs
F>M
History
Non-Arteritic (NAAION)
Vascular risk factors
No pain
Arteritic (AAION)
May have preceding amaurosis fugax
“GCA” symptoms
Visual Loss
Non-Arteritic (NAAION)
Less severe (mean 6 / 30)
Arteritic (AAION)
More severe (mean CF)
Optic Disc
Non-Arteritic (NAAION)
Sectoral swelling (often superior)
“Disc at risk”
Arteritic (AAION)
Chalky-white (more pallor)
Diffuse swelling
Later cupping
Prognosis
Non-Arteritic (NAAION)
Better
Arteritic (AAION)
Worse
Investigations
Non-Arteritic (NAAION)
Vascular risk factors
Overnight sleep study
Arteritic (AAION)
↑ ESR / CRP
(FFA: severe choroidal hypoperfusion)
⊕ Temporal artery biopsy
Management
Non-Arteritic (NAAION)
No proven treatment
Arteritic (AAION)
Systemic steroids
i. Pseudo
- Optic disc drusen
- Pseudophakia
- Myelinated nerve fibre layer
- Optic nerve hypoplasia, disc pit
ii. Real
A) Primary
Without preceding swelling of the optic disc
- Following retrobulbar optic neuritis, posterior ischaemic optic neuropathy
- Compression (tumour, aneurysm), traumatic optic neuropathy
- Hereditary optic neuropathy, retinal dystrophies (e.g. retinitis pigmentosa)
- Nutritional optic neuropathy (e.g. B12, folate)
- Drug-induced optic neuropathy (e.g. ethambutol, isoniazid, amiodarone, vigabatrin)
- Radiation
Pale, flat, well delineated disc
B) Secondary
With preceding swelling of the optic disc
See below - Optic Disc Swelling
White, raised, poorly delineated disc
Pale, flat, well delineated disc
White, raised, poorly delineated disc
“ATROPHIC M”
- Advanced glaucoma
- Traumatic, toxic
- Radiation, retinal
- Optic neuritis (demyelinating, infectious, inflammatory, infiltrative)
- Papilloedema, paraneoplastic
- Hereditary
- Ischaemic
- Compressive
- Metabolic (DM, MPS)
- Physiological +
- Glaucomatous
- Non-glaucomatous
- Congenital (optic disc pit, myopia)
- Compression
- Arteritic Anterior Ischaemic Optic Neuropathy
- Toxic (methanol)
Red flags for Non-Glaucomatous Cupping
- Acute change in symptoms / signs
- Vision
- ↓ Visual acuity
- Redness / brightness
- Colour vision
- ON
- Pallor of the rim
- Asymmetry
- HVF
- Vertical / junctional defect
- Asymmetry
- Doesn’t correlate with disc
Previous
7.9 Nystagmus
Next
8.0 Introduction
All rights reserved. No part of this publication which includes all images and diagrams may be reproduced, distributed, or transmitted in any form or by any means, including photocopying, recording, or other electronic or mechanical methods, without the prior written permission of the authors, except in the case of brief quotations embodied in critical reviews and certain other noncommercial uses permitted by copyright law.
Vitreoretinal Surgery Online
This open-source textbook provides step-by-step instructions for the full spectrum of vitreoretinal surgical procedures. An international collaboration from over 90 authors worldwide, this text is rich in high quality videos and illustrations.